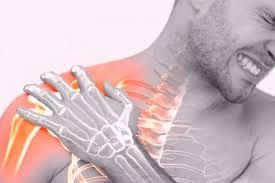
Understanding the Shoulder’s “Double Trouble” Problem
Many people are surprised to learn that a painful rotator cuff tear can sometimes lead to a frozen shoulder.
At first, it seems like the shoulder injury simply hurts… but over time, the shoulder doesn’t just hurt — it becomes stiff, hard to move, and “stuck.”
So what happened?
Let’s walk through how this progression can occur.
First — What Is the Rotator Cuff?
The rotator cuff is a group of four muscles and tendons that surround the shoulder joint. Their job is to:
- Stabilize the ball-and-socket joint
- Help lift and rotate the arm
- Keep the shoulder moving smoothly
The most commonly injured tendon is the supraspinatus, which helps lift the arm out to the side.
Rotator cuff tears can happen from:
- Wear and tear with age
- Repetitive overhead activity
- Sports like pickleball, tennis, or golf
- Falls or sudden lifting injuries
When the cuff tears, people often feel:
- Pain lifting the arm
- Weakness
- Night pain (especially lying on that side)
- A painful arc of movement
At this stage, the shoulder is painful — but still movable.
Step One — Pain Changes Movement
Here’s where the story begins to shift.
Because movement hurts, people naturally start protecting the shoulder.
They may:
- Stop reaching overhead
- Avoid putting on jackets or bras
- Limit rotation movements
- Keep the arm tucked close to the body
- Sleep without moving the shoulder
This protective behavior is completely understandable — but it comes at a cost.
The shoulder joint is designed to move frequently. When it doesn’t, the joint environment starts to change.
Step Two — The Shoulder Becomes Inflamed
A rotator cuff tear doesn’t just affect the tendon.
It often creates irritation in surrounding structures, including:
- The subacromial bursa
- The joint lining (synovium)
- The capsule that surrounds the joint
Inflammation causes:
- Swelling
- Increased fluid
- Chemical irritation
- Pain with movement
If this inflammatory state continues — especially with reduced movement — the joint capsule itself can become involved.
Step Three — The Capsule Tightens
The shoulder joint is surrounded by a loose connective tissue sleeve called the joint capsule.
Its job is to allow large ranges of motion while keeping the joint stable.
When inflamed, the capsule can begin to:
- Thicken
- Tighten
- Develop adhesions (scar-like tissue)
- Lose elasticity
This process is called adhesive capsulitis — better known as frozen shoulder.
Once this begins, the problem is no longer just the rotator cuff. Now the entire joint is stiff.
Step Four — Motion Becomes Mechanically Blocked
Early on, movement is limited by pain.
Later, it’s limited by stiffness.
Patients often say:
“At first it hurt to move… now it just won’t move.”
This is a key transition point.
Frozen shoulder follows a classic pattern of motion loss:
- External rotation (turning arm outward) is most limited
- Abduction (lifting arm sideways) becomes restricted
- Internal rotation (reaching behind back) tightens
Even if pain improves, stiffness can continue progressing.
The Vicious Cycle
Once stiffness begins, it reinforces itself.
Here’s the cycle:
Rotator cuff tear → Pain → Less movement → Inflammation → Capsular tightening → More stiffness → More pain → Even less movement
Over time, patients may lose the ability to:
- Reach overhead
- Wash their hair
- Fasten a bra
- Reach into the back seat
- Sleep comfortably
At this stage, the shoulder often feels “frozen.”
Who Is More Likely to Develop Frozen Shoulder?
Not every cuff tear leads to frozen shoulder — but some people are at higher risk.
These include:
- Women aged 45–65
- People with diabetes
- Thyroid disorders
- Post-surgical shoulders
- Shoulders immobilized in slings
- High pain sensitivity leading to guarding
Often patients describe the timeline like this:
“It started as shoulder pain… then over months it just froze up.”
The Timeline of Progression
While everyone is different, a typical pattern may look like:
0–6 weeks
Painful rotator cuff phase
6–12 weeks
Guarding and reduced movement
3–6 months
Freezing phase (inflammation + stiffness)
6–18 months
Frozen → gradual thawing phases
Frozen shoulder can take 1–2 years to fully resolve if not treated early.
Why Early Treatment Matters
The good news? Early physiotherapy can significantly reduce the risk of a cuff tear progressing into frozen shoulder.
Treatment focuses on:
- Maintaining gentle range of motion
- Reducing inflammation
- Protecting the tendon while keeping the capsule mobile
- Preventing scar tissue formation
Early exercises may include:
- Pendulum swings
- Assisted arm lifts
- Table slides
- Gentle external rotation stretches
The goal is simple: Keep the shoulder moving safely — even while it heals.
Key Takeaway
A rotator cuff tear and frozen shoulder are different problems — but they can become connected.
If shoulder pain leads to prolonged guarding and immobility, the joint capsule can tighten and scar, creating a second condition layered on top of the first.
That’s why early assessment and guided treatment matter.
Addressing cuff pain early can help prevent months — or even years — of stiffness later.